Treatment of venereal diseases
Sexually Transmitted Diseases (STDs)
Sexually transmitted diseases (STDs) are infections that are transmitted from one person to another through sexual contact. The causes of STDs are bacteria, parasites and viruses. There are more than 20 types of STDs, including
- Chlamydia
- genital herpes
- HPV
- trichomoniasis
- etc
Analyzing the most common
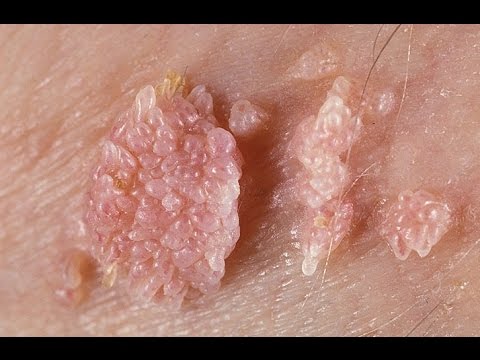
Acute Warts
What are warts?
Warts are the most common sexually transmitted disease. The use of a condom does not exclude the transmission of the virus, 50% of sexually active people will be infected with the HPV virus at some point. Warts will appear in only 10% of them, as the virus is fought by the immune system and does not manifest, remaining latent condition.
HPV viruses 16,18,31,45 are considered to be the highest risk subtypes responsible for various malformations, especially cervical cancer, while the low risk viruses that are mainly responsible for warts are HPV 6, 11, 42 , and 44.
The types of HPV6 & amp; HPV11 is responsible for 90% of warts.
Although warts can be removed from the affected area, the HPV virus stays in the body forever.
Symptoms
Warts in women occur in the area of the vagina, cervix, small and large lips, urethra and more rarely in the bladder. Causes that help warts grow are infections, vaginal discharge and pregnancy. In pregnancy, warts can spread very easily.
In men, they occur on the foreskin, body of the penis, scrotum, pubic area, foreskin, and urethra. Topics that help acute warts develop include topical corticosteroids, urethritis, gout, immunosuppression (eg HIV infection) and diabetes.
Warts do not cause discomfort and therefore may not be noticeable by the patient, they are pink or rarely brown in color, soft with a smooth, or wavy surface and a broad or scaly base. They are transferred from one area to another and can join in larger lesions.
Warts occur in both the anus and the pharynx.
In addition to warts, high-risk hpv infections can lead to precancerous lesions in both men and women.
These lesions are often found together with wart lesions and to a significant extent can lead to cancer in the respective areas.
A woman who has warts does not mean that she will develop cervical cancer.
Mild complications of warts are erosions and wounds to the skin and mucous membranes, bleeding, inflammation, and problems urinating and defecation. Also very important are the psychological problems that result from HPV infection. anus, even the intestine.
Prevention
The only way to prevent warts is monogamy, as even the use of a condom does not completely protect against the HPV virus. Circumcision in men significantly helps reduce the risk of transmitting the virus and the chances of infection. There are also two vaccines for HPV. Gardasil is specific for HPV16, 18, 6, 11. Cervarix protects against 16.18 which are responsible for neoplasms and cervical malformations. Both of these vaccines are preventive and not therapeutic. It is recommended to be done before the beginning of sexual life, in order to effectively protect against warts and neoplasms of the cervix. The diagnosis of warts is made clinically by an experienced dermatologist who will suggest the appropriate treatment.
Genital herpes
What is genital herpes?
Genital herpes is a genital herpes infection caused by the herpes simplex virus (HSV). Most people who are carriers of the disease do not know they are infected and many will never develop the disease, with the typical small blisters. Although there is no cure for the disease, over time the symptoms are milder and the manifestations are increasingly rare. When it is symptomatic, the typical manifestation of the primary infection of the genital area are inflamed papules and blisters on the outer surface of the genitals.They usually appear 4-7 days after the first sexual exposure to HSV. The herpes simplex virus HSV is classified into two distinct categories, HSV-1 and HSV-2. HSV-1 subtype causes about one-sixth of genital infections, and the rest is due to HSV-2.
Genital herpes - Clinical picture
In men, lesions occur on the glans penis, the body of the penis or other parts of the genital area, the inner surface of the thighs, the buttocks, or the anus. In women, the lesions appear on or near the genital area, clitoris or other parts of the vulva, buttocks or anus. Other common symptoms include pain, itching, and burning. Less common symptoms are discharge from the penis or vagina, fever, headache, muscle aches (myalgia), swollen lymph nodes and malaise. Women often experience additional symptoms including painful urination (dysuria) and cervicitis. Herpetic proctitis (inflammation of the anus and rectum) is common in people involved in anal intercourse. After 2-3 weeks, the existing lesions develop into ulcers and then a crust forms and the lesions heal. If they are in the mucosa they may never form a crust.
Relapses
After about 80% of the first episodes of genital herpes caused by HSV-2, there will be at least one relapse, with the recurrence rate for genital herpes caused by HSV-1 is about 50%. Genital herpes caused by HSV-2 recurrs on average four to six times a year, while that of HSV-1 infection occurs only once a year. People with recurrent genital herpes can be treated with suppressive antiviral therapy using acyclovir, valacyclovir or famciclovir.Suppressive therapy is useful in those who have at least four relapses per year. People with lower relapse rates will also have fewer relapses with sedative therapy. Sedative treatment should be discontinued after a maximum period of one year and the recurrence rate reassessed. Diagnosis is usually made clinically after examination by a dermatologist. Also culturing the virus from bubble fluid will give the definitive diagnosis. Hematologically, one can detect the presence of antibodies (ie carriers of the virus) to the herpes simplex virus type I (HSV-1) or type 2 (HSV-2).
Genital herpes - Treatment
There is no cure for genital herpes. It can be transmitted before and after the onset of symptoms. But antiviral drugs can shorten the effects. These drugs include acyclovir, valaciclovir, and famciclovir. Acyclovir is an antiviral drug used against herpes viruses, chickenpox, shingles, and Epstein-Barr viruses. This medicine reduces the pain and the number of lesions in the initial manifestation of genital herpes. In addition it reduces the frequency and severity of relapses. Valacyclovir is also used to treat herpes virus infections. Inside the body, it is converted to acyclovir. Helps relieve pain and suffering and makes wounds heal faster.
Urethritis-Vaginitis
Gonococcal (specific urethritis)
1) High infectivity
2) Short incubation time
3) Lack of non-infectious space
4) High rates of asymptomatic patients (men 2-5%, women 40-50%)
Ways of transmission
The most common sexually transmitted disease worldwide after infections with hair follicles, chlamydia, HPV, is transmitted through sexual contact.
From man to woman more often (80%, vice versa 20%), contact with contaminated objects (eg toilet)
Childbirth: Gonococcal eye (formerly most common causes of blindness)
Clinical picture in man
Apparent automatic purulent secretion of viscous creamy yellow-yellow-green pus (traitor stains on underwear), dysuria.
Erythematous and edematous mouth of the urethra in gagging can also cause balanoposthitis.
Without treatment or with mechanical factors (eg riding a motorcycle), discharge and posterior urethritis with more severe symptoms, hematuria, fever, arthralgia, usually after 6 months asymptomatic. In homosexuals, a single rectal infection with little discharge and sometimes bleeding.
Complications in the man
Paraurethritis (pain in the scapular cavity)
Pureuritis, periurethral fibrosis and stenoses.
Periurethral abscess with fistula.
Prostatitis (10% of gonococcal etiology), In the acute phase fever, feeling sick, pseudo-abscess. In chronic prostatitis dysuria, incomplete emptying of the bladder, burning sensation in the urethra, pain in the lower abdomen.
Epididymitis (15% gonococcal etiology), fever, severe vaginal pain which appears red and swollen. The discharge is often absent, the testicles are not affected, resulting in narrowings with oligospermia in unilateral and azoospermia in bilateral infection,sterility.
Inflammation of the bulbar urethra with perineal pain, foreign body sensation in the anus and fistulas.
Clinical picture in woman
Acute gonorrhea: 50% asymptomatic or mild symptoms, risk of chronic disease.
In contrast to the man simultaneous onset in several places: urethritis, cervicitis, proctitis.
Increased vaginal discharge, dysuria, lower abdominal pain.
Menorrhagia, irregular menstruation when the endometrium is affected
Complications in women
From the endometrium to the fallopian tubes and from there to the ovaries, pelvis and peritoneum.
Bartholonitis: painful nodules on the large lips of the vulva, swelling and erythema in small lesions usually unilateral, difficult walking.
Mucus secretion from the bartholin glands and periurethral glands, obstruction and abscess with fistula in the vagina
Cystitis (dysuria)
Salpingitis, PID σ10% of cases, most common causeinfertility in the third world. Gonorrheal peripatitis with symptoms similar to acute cholecystitis (usually from Chlamydiatrachomatis). Laparoscopically characteristic adhesions in the form of violin strings. Chronic urethritis: Minimal to no symptoms. Chlamydia must be ruled out, so cultivation is essential. Significant complications: chronic appendicitis with abdominal pain, fever, cycle abnormalities, adhesions, fallopian tubes, infertility. Non-specific urethritis In the past rare today 10 times more common than gonorrhea, the most common contact-transmitted infection of the genital area.


